Left Lung Removal Doesn’t Slow Cancer Survivor
| Brad Welch, 57, doesn’t look or act like a lung cancer survivor who had his entire left lung removed just six months ago.
Welch, of Conway, has been clearing brush, deer hunting and exercising just as he did before his cancer surgery.
He got his life back, he said, because he made it a priority to get to the University of Arkansas for Medical Sciences (UAMS) Winthrop P. Rockefeller Cancer Institute.
In addition to his lung cancer diagnosis, he was told by his local doctor that he had emphysema and COPD (chronic obstructive pulmonary disease) and that he needed to improve his lung function for eventual chemotherapy.
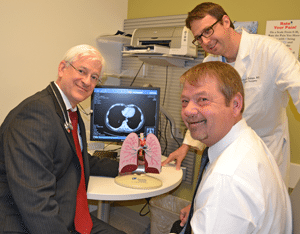
Thaddeus Bartter, M.D., (seated, left) and Matthew Steliga, M.D., (standing) reviewed Brad Welch’s left lung removal during a recent follow-up visit.
“I wasn’t told verbatim that it was inoperable, but that was the message I got,” Welch said. “At that point I knew I needed to be seen at UAMS because I had already researched it online and knew that was the best place to go if you have cancer.”
Welch, a distribution designer for Entergy Arkansas, gathered his medical records and headed to UAMS. On his first visit he was seen by two key members of UAMS’ lung cancer team: Thaddeus Bartter, M.D., an interventional pulmonologist who performs patient evaluations and diagnoses, and Matthew Steliga, M.D., a cardiothoracic surgeon with advanced training in the removal of cancers of the chest, primarily lung cancer.
Bartter examined Welch’s airways by performing an endobronchial ultrasound. This test creates images of the lungs using a bronchoscope, which is passed through the mouth and down the windpipe to the lungs. The bronchoscope also is used to biopsy the tumor. To determine if the cancer had spread outside Welch’s lung, Bartter requested a PET scan, the most sophisticated imaging available for cancer detection.
His tests at UAMS revealed some surprisingly good news: The cancer was confined to his left lung, and he did not have COPD or emphysema, so Welch’s overall lung function was otherwise OK.
This meant that Welch was a good candidate for surgery to remove the cancer, which is the best chance for a cure. Welch had squamous cell lung cancer, a form of non-small cell lung cancer, which is slower growing than some other types of lung cancer.
“We were fortunate to find Mr. Welch’s tumor when it was localized to the lung,” Steliga said. “Most patients with lung cancer get to the doctor at a stage when it has already spread. At that point, they’ve unfortunately missed the best chance for surgery.”
The only catch for Welch was that the location and size of his cancer meant his entire left lung would have to be removed. While the surgery is not common in many places, it’s familiar territory for UAMS’ lung cancer team.
“It’s a common operation that we do here often, but it’s a big surgery to go through and not all patients are strong enough to tolerate that type of operation,” Steliga said.
Before proceeding with the surgery recommendation, a consensus was reached by the lung cancer team, which in addition to interventional pulmonary medicine and thoracic surgery includes doctors in interventional radiology, medical oncology and radiation oncology.
“The team meets each week on every lung cancer patient and considers treatment options from every different perspective or approach,” Steliga said. “We all get together in one place and review the data and form a conclusion. With each case we always come to a good conclusion of what is the safest, best approach for each patient.”
Welch said he researched the lung team’s recommendation to remove his left lung and agreed to have the surgery. His positive hospital stay was punctuated by the care he received from Teka Bartter, a UAMS advanced practice nurse and lung cancer coordinator.
“She was amazing coordinating information when I needed it, answering questions between doctor visits, and even following up during my recovery at home,” Welch said.
Within a few weeks after surgery he was walking more than a mile a day. He returned to work full time in 12 weeks.
“I’ve been deer hunting, clearing brush, exercising 30 minutes every day,” Welch said. “I can’t tell a bit of difference in my quality of life. I can’t tell you how pleased I am and I owe it all to Dr. Steliga and Dr. Bartter.”
“He went from being told he didn’t have a chance to being cancer free,” Bartter said. “He looks fantastic.”