View Larger Image
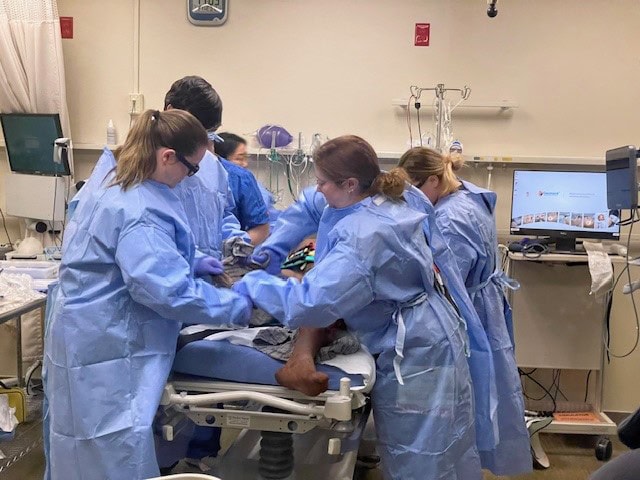
Interprofessional students assess a patient who was just wheeled in.
Interprofessional UAMS Students Monitored for Stress During Trauma Simulation
| A man whose right leg was severed below the knee, leaving a jagged and bloody bone fragment sticking out of his pants leg, was surrounded by people in blue scrubs as paramedics wheeled him into a trauma bay at the University of Arkansas for Medical Sciences (UAMS) on a recent morning.
The blue-clad workers — surgical residents and nursing students — quickly encircled the patient to check his vital signs as Joseph Margolick, M.D., a general and trauma surgeon, scribbled information on a dry-erase board on the wall.
Paramedics and emergency medical technicians from Metropolitan Emergency Medical Services (MEMS), who unloaded the patient from the ambulance just outside the door, said he had been extricated from a vehicle after an automobile accident. In addition to the severed leg, the patient had a large gash on his forehead above his right eye, a gaping wound on his abdomen and blood seeping out from underneath him.
Even though the small group of trainees knew the patient was a manikin and the situation a simulation, their actions were closely monitored, because in this scenario, they were the primary focus of the exercise as they monitored his blood pressure, reviewed X-rays and communicated with one another.
To make the situation more real, the manikin was a “high-fidelity” model supplied by MEMS, which obtained it as part of a grant award.

Paramedics prepare to wheel a manikin representing an automobile accident patient into the trauma bay.
Not only did the manikin’s skin look and feel like that of an actual person but it also could mimic some human body functions, such as pulsating blood, heaving chest movements and breathing sounds. Capt. Cody Hughes, a MEMS paramedic and instructor for the simulation, said the manikins are even designed to bleed out or die if a crucial diagnosis is missed, which increases the likelihood of panic during simulations.
Karen Dickinson, M.D., an assistant professor of surgery at UAMS and director of interprofessional simulation and clinical skills training, said that in addition to the educational component of this simulation, her research work is examining the stress response of interprofessional students within trauma simulations.
“In order to comprehensively measure human stress, these interprofessional participants had multiple markers of stress measured, including blood pressure, biochemical markers, speech pattern, and psychological assessment through a questionnaire,” Dickinson said.
Dickinson said the results from the stress markers taken during the educational session will be analyzed for purposes of understanding the effects of trauma training on health care students.
“In simulation, you want to provide a psychologically safe environment, but you also need a certain level of stress to simulate real life,” Dickinson said. “We want to assess interprofessional learners’ stress, as well as identifying ways to mitigate it. We will use these observations to optimize learning at UAMS.”
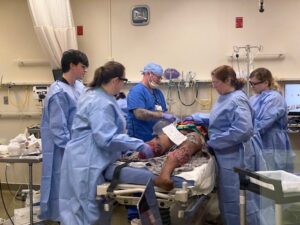
Interprofessional UAMS students are monitored for stress as they attempt to stabilize the patient before transferring him to the operating room.
After the group in blue scrubs stabilized the patient and transferred him to the Operating Room, they gathered in a room in the UAMS Simulation Center to discuss the experience. Dickinson and Margolick debriefed the learners, asking how they felt during the simulated emergency and what they thought about the level of communication, direction and leadership during the exercise.
Also participating as a facilitator in the interprofessional debrief session, Hughes encouraged the learners to feel free to ask paramedics more questions when patient is brought in to optimize patient care.
“We’ve been with the patient for 10 or 20 minutes,” Hughes said. “Maybe he was talking to me before becoming unconscious.”
Margolick said the participation of the fully trained EMTs and paramedics, who practiced critical prehospital maneuvers including bleeding cessation and vehicle extraction, helped foster teamwork between themselves and the UAMS Emergency Department and trauma team.
Throughout the day, three groups of seven to eight learners at a time participated in similar back-to-back sessions, ensuring that many learners could be trained and generate a good amount of data regarding human stress to analyze.